Your Daily Meds - 25 November, 2022
Good morning and welcome to your Friday dose of Your Daily Meds.
Bonus Review: Are there any differences in composition between interstitial fluid and lymph?
Answer: Nope. Not really.
Lymph is just interstitial fluid that has entered the lymphatic channels.
Thoracic duct lymph will have a higher protein concentration than most of the body’s interstitial fluid due to the drainage of protein-rich hepatic lymph (interstitial fluid) into the thoracic duct.
A Query:
Which of the following is not considered a risk factor for preeclampsia?
Past history of preeclampsia
Maternal hypertension
Maternal insulin resistance
Chronic kidney disease
Multiparity
Have a think.
Scroll for the chat.
A Case:
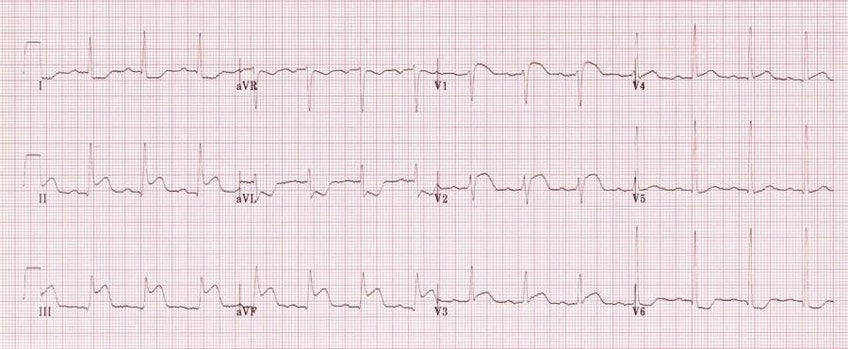
A 65-year-old male presented to the Emergency Department with chest pain and diaphoresis. His BP dropped to 90/60 following administration of sublingual nitrates in the ED. His ECG is shown below:
Which of the following correctly describes the most likely diagnosis?
Inferior infarction
Anterior infarction
Lateral infarction
Supraventricular tachycardia
Mobitz II heart block
Have a think.
Scroll for the chat.
Mind the Gap:
Preeclampsia is a disorder characterised by the new onset of hypertension and proteinuria or significant end-organ dysfunction in the last half or pregnancy or in the post-partum period. Preeclampsia is caused by a disordered placental and maternal vascular function that always resolves after delivery of the child.
A past history of preeclampsia, pre-existing maternal hypertension, pre-gestational diabetes and chronic kidney disease are all risk factors for the development of preeclampsia.
Multiparity is not considered a risk factor for the development of preeclampsia. Conversely, nulliparity, or first pregnancy, is considered a risk factor, with the theory being that the nulliparous maternal immune system has limited exposure to paternal antigens, and that the lack of sensitisation may play a role in preeclampsia development.
Squiggly Death Lines:
This ECG shows sinus rhythm at a rate or approximately 80 bpm. There are signs of an inferior ST-elevation myocardial infarction (STEMI) with ST-segment elevation in the inferior leads II, III and aVF. There is also reciprocal ST-segment depression in the lateral leads of I, aVL and V6.
This patient was eventually diagnosed with a right ventricle infarction after ST-segment elevation was noted on a right-sided V4 chest lead. Patients with right ventricular infarction are preload sensitive which may explain this man’s exaggerated hypotensive response to sublingual nitrates.
An anterior infarction is more likely to show ST-segment changes on the praecordial leads V2-4 and lateral infarction may show more significant changes in the lateral leads such as V5-6, I and aVL.
A Mobitz II heart block is a type of 2nd degree AV block characterised by non-conducted P waves without progressive elongation of the PR interval.
Head to the ‘Life In The Fast Lane’ site for more of this goodness.
FOAMED Friday:
RSV Bronchiolitis
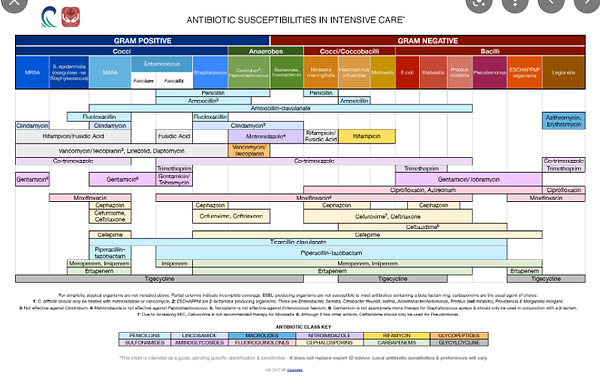
Antibiogram
Note: This is from Wellington, New Zealand, from memory - so there will always be some local differences in susceptibilities but is is an excellent guide. So click the link and click through to download the high quality PDF, then save it to the notes app on your phone. Thanks me later…
News: I made a little Ward Call Course for you all. It maps out an Evening Ward Call shift and covers a bunch of common tasks that you may need to do, like:
Deteriorating Patients
Heparin Infusions
Fluid Orders
Electrolyte Replacement
Difficult patients - Discharge Against Medical Advice, Ryan’s Rule
End of Life etc
You can find the course page here:
It’s free and always will be. Let me know what you think.
Remember, you are free to rip these questions and answers and use them for your own flashcards, study and question banks.
As always, please contact me with any questions, concerns, tips or suggestions. Have a great day!
Luke.